Tiazac ®

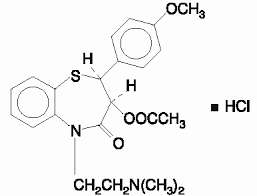
Diltiazem
Diltiazem is metabolized by and acts as an inhibitor of the CYP3A4 enzyme.
Mechanism
Diltiazem is a potent vasodilator, increasing blood flow and variably decreasing the heart rate via strong depression of A-V node conduction. Its pharmacological activity is somewhat similar to verapamil.[2]
Potent vasodilator of coronary vessels.
Vasodilator of peripheral vessels. This reduces peripheral resistance and afterload.
Negative inotropic effect. Diltiazem causes a modest decrease in heart muscle contractility and reduces myocardium oxygen consumption.
Negative chronotropic effect. Diltiazem causes a modest lowering of heart rate. This effect is due to slowing of the SA (sinoatrial) node. It results in reduced myocardium oxygen consumption.
Negative dromotropic effect. By slowing conduction through the AV (atrioventricular) node, diltiazem increases the time needed for each beat. This results in reduced myocardium oxygen consumption by the body.
Nontherapeutic effects and toxicities
Reflex sympathetic response. Caused by the peripheral dilation of vessels and the resulting drop in BP; the response works to counteract the negative inotropic, chronotropic and dromotropic effects of diltiazem. Undesirable effects of Diltiazem include hypotension, bradycardia, dizziness, flushing.[3]
Indications
Angina:
· Stable angina (exercise-induced) . Diltiazem increases coronary blood flow and decreases myocardial oxygen consumption, secondary to decreased peripheral resistance, heart rate, and contractility.[4][5]
· Variant angina. Diltiazem is effective due to its direct effects on coronary dilation.
· Unstable angina (preinfarction, crescendo). Diltiazem may be particularly effective if the underlying mechanism is vasospasm.
Hypertension. Because of its vasodilatory effects, diltiazem is useful for treating hypertension. Calcium channel blockers are well-tolerated, and especially effective in treating low-renin hypertension.[8]
Contraindications and precautions
CHF. Patients with reduced ventricular function may not be able to counteract the inotropic and chronotropic effects of diltiazem, the result being an even higher compromise of function.
SA node or AV conduction disturbances. Use of diltiazem should be avoided in patients with SA or AV nodal abnormalities, because of its negative chronotropic and dromotropic effects Low blood pressure. Patients with systolic blood pressures below 90 mm Hg should not be treated with diltiazem.
Wolff-Parkinson-White syndrome. Diltiazem may paradoxically increase ventricular rate in patients with WPW syndrome because of accessory conduction pathways.
Drug interactions
Beta-blockers
Intravenous diltiazem should be used with caution with beta-blockers, because while the combination is most therauputically beneficial, there are rare instances of dysrhythmia and AV node block [9].
Quinidine
Quinidine should not be used concurrently with calcium channel blockers because of reduced clearance of both drugs and potential pharmacodynamic effects at the SA and AV nodes.
Miscellaneous
Inhibition of hepatic enzymes. Diltiazem and verapamil inhibit hepatic cytochromes CYP3A4, CYP2C9 and CYP2D6, possibly resulting in drug interactions.
Potential future indications
Diltiazem is also being used in the treatment of anal fissures. It can be taken orally or applied topically with equal effectiveness. When applied topically, it is made into a cream form using either vaseline or Phlogel. Phlogel absorbs the diltiazem into the problem area better than the vaseline base. It has good short term success rates. [14][15] Like all non-surgical treatments of anal fissure it does not address the long term problem of increased basal anal tone and does not decrease the subsequent recurrence rate that can vary between 40 to 60%.